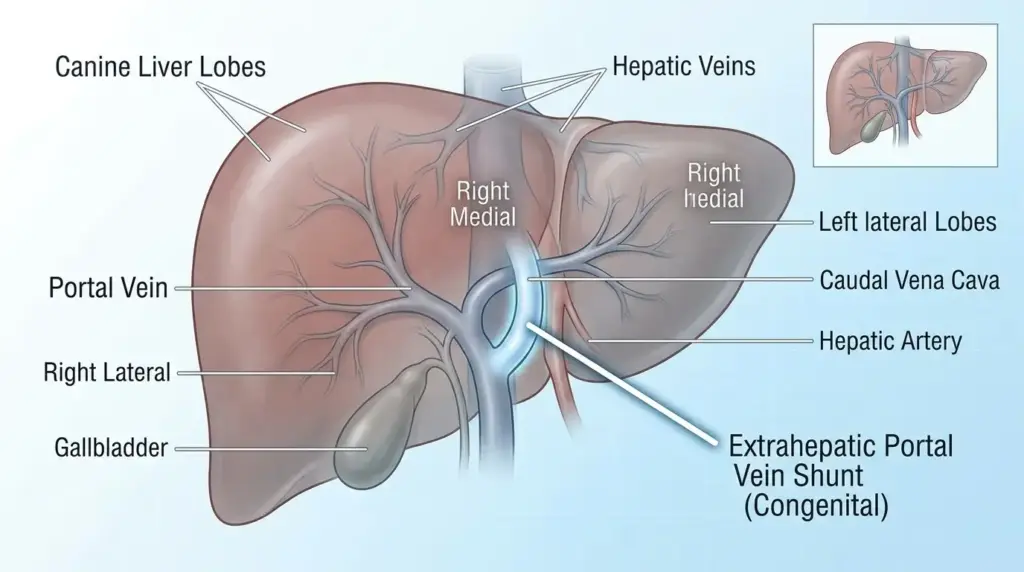
A diagnosis of a liver shunt is a heavy hit for any puppy owner, but understanding the mechanics of the condition is the first step toward recovery. Formally known as a portosystemic shunt (PSS), this anatomical defect involves an abnormal connection that allows blood from the dog’s gastrointestinal tract to bypass the liver. Instead of being filtered for toxins and processed for nutrients, this blood enters the systemic circulation directly.
Statistically, about 80% of liver shunts in dogs are congenital, meaning the puppy is born with the defect. In the womb, a vessel called the ductus venosus naturally shunts blood around the non-functional fetal liver. Under normal conditions, this vessel collapses shortly after birth to allow the liver to take over its metabolic duties. When it fails to close, the puppy is left with a functional “leak” in their circulatory system.
Identifying the Signs: Neurological and Physical Symptoms
Because the liver is responsible for filtering out metabolic byproducts like ammonia, a shunt leads to a buildup of toxins in the bloodstream. This often manifests as hepatic encephalopathy—neurological symptoms that can be frightening to witness. Owners often report “head pressing,” where a dog stands in a corner and pushes its forehead against the wall, or aimless circling and disorientation. In severe cases, this progresses to seizures.
Physical growth is also affected. Puppies with shunts are typically the “runts” of the litter, appearing smaller and less active than their siblings. You might also notice gastrointestinal issues like vomiting or diarrhea, particularly after a high-protein meal, as the body struggles with the resulting metabolites. Some dogs even develop bladder stones or pica (eating non-food items) due to the metabolic imbalance.
The Diagnostic Path: From Bloodwork to Advanced Imaging
Diagnosing a shunt requires a systematic approach. Initial blood chemistry panels often show low levels of blood urea nitrogen (BUN) and albumin, along with elevated liver enzymes like ALT and AST. A urinalysis might reveal ammonium biurate crystals, which are a strong indicator of liver dysfunction.
The definitive non-invasive test is the bile acid test. This requires two samples: a fasting baseline and a second sample taken after a meal. A significant spike in bile acids suggests the blood is not being properly processed by the liver. To pinpoint the shunt’s location, veterinarians use ultrasound with contrast, CT scans, or MRIs. Recent research from Cornell University suggests that many intrahepatic shunts (those inside the liver) are actually located between liver lobes rather than deep within the tissue, which influences surgical options.
Treatment Protocols: Surgery vs. Medical Management
Surgery is the gold standard for extrahepatic shunts (those outside the liver). Modern techniques rarely involve closing the shunt all at once, as the sudden increase in blood pressure (portal hypertension) can be fatal. Instead, surgeons use ameroid constrictors or cellophane bands that gradually close the vessel over several weeks, giving the liver time to adapt to the increased blood flow.
For mild cases or complex intrahepatic shunts where surgery isn’t viable, medical management is the fallback. This focuses on reducing toxin production in the gut. Lactulose is frequently prescribed as a synthetic sugar that acts as an osmotic laxative, speeding up transit time to minimize ammonia absorption. Diet also plays a massive role; these dogs require high-quality, highly digestible proteins—often plant or dairy-based—to keep the liver’s workload manageable. While medical therapy can provide a decent quality of life, these dogs should never be bred due to the clear genetic component of the condition.